In this episode, I’ll discuss a Monte Carlo analysis I performed to assess the risk of anesthetic awareness when giving rocuronium before ketamine (rocketamine) in rapid sequence intubation.
Background
Recently, Dr. Josh Farkas at pulmcrit.org wrote an excellent post discussing whether in certain scenarios rocuronium should be administered before ketamine in rapid sequence intubation. This is the reverse of the more common RSI practice of giving the sedative followed by the paralytic.
In his post, Josh uses the example of a morbidly obese patient with hypoxic respiratory failure and an oxygen saturation of 96% despite maximal preoxygenation efforts. Such a patient has a very short “safe apnea time” of perhaps 2 minutes, beyond which if their airway is not secure they will likely suffer anoxic injury.
With the traditional approach of giving ketamine before rocuronium, Josh estimates a 1 minute “sedation lag time” where the ketamine will kick in before the rocuronium. This is problematic because the patient may become apneic from a fast ketamine push 1 minute before the intubating conditions are rendered ideal by rocuronium. In this scenario, 50% of the safe apnea time is used up waiting for the rocuronium to work, leaving the physician with a very narrow window of time to place the airway without a risk of anoxic injury.
By reversing the usual order and giving rocuronium first, Josh points out that this sedation lag time should be minimized, assuming an onset of 50-60 seconds for rocuronium, an onset of 30-40 seconds for ketamine, and a few seconds to complete the administration of each drug.
As some comments in Josh’s post point out, these onset times for rocuronium and ketamine are only averages – there are standard deviations that may make a difference in the calculation of the sedation lag time.
The major risk that comes from giving rocuronium before ketamine is the risk of “anesthetic awareness.” That is, the risk the rocuronium kicks in before the ketamine does and the patient is paralyzed but not yet sedated.
To determine the risk of anesthetic awareness from pushing rocuronium before ketamine, I performed a Monte Carlo analysis using 5000 simulated patients.
Methods
In one of the most commonly cited papers comparing the onset of rocuronium to succinylcholine, the average onset of paralysis from rocuronium 1.2 mg/kg IV was 55 seconds with a standard deviation of 14 seconds.
In a separate study, the onset of ketamine 2mg/kg IV was 46.05 seconds with a standard deviation of 1.93 seconds.
To assess the risk of anesthetic awareness, I simulated the onset times for ketamine and rocuronium 5000 times using Microsoft Excel to create random values with a normal distribution around each mean onset time.
I assumed that each medication would be given sequentially and that administration would take 20 seconds for each medication. I then calculated the sedation lag time and anesthetic awareness time for each simulated patient receiving rocuronium first and again receiving ketamine first.
Results
When ketamine was given first, the average sedation lag time was 49 seconds. In a patient with a 2 minute safe apnea time, this represents 41% of the safe apnea time used up waiting for medications to work.
One out of 5000 simulated patients had a 3.9 second period of anesthetic awareness. However, this simulated value had rocuronium taking effect at 4 seconds after administration.
When rocuronium was given first, the sedation lag time was 15.1 seconds in simulated patients without an episode of anesthetic awareness. In a patient with a 2 minute safe apnea time, this represents 13% of the safe apnea time used up waiting for medications to work.
25.3% of simulated patients had some duration of anesthetic awareness. 15.4% of simulated patients had an anesthetic awareness time greater than 5 seconds, 8.9% had an anesthetic awareness time greater than 10 seconds, 2.2% had an anesthetic awareness time greater than 20 seconds, and 0.4% had an anesthetic awareness time greater than 30 seconds.
Discussion
The validity of this analysis is limited because I used onset times from two different patient populations, neither of which were critically ill. Perfusion of muscles (which is poor to begin with) is worse in critically ill patients with shock, and this would extend the onset of rocuronium. In turn, the risk of anesthetic awareness with rocuronium first would be lower and the sedation lag time would be higher with ketamine first.
Two-thirds of the simulated patients that experienced anesthetic awareness would not have if the administration time of ketamine were shortened to 10 seconds. Such a rapid administration time of ketamine has a greater chance of causing apnea.
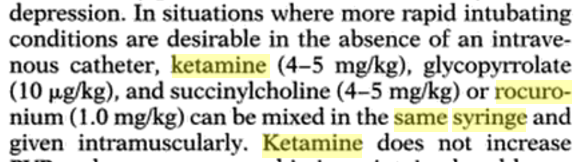
If ketamine and rocuronium were mixed in the same syringe, the risk of anesthetic awareness would be 2.2%. Unfortunately, no published data examines the stability of rocuronium and ketamine in the same syringe. There are two textbooks which state that ketamine and rocuronium may be mixed in the same syringe however they provide no citation for this claim (click through the images to the book):
Conclusion
The risk of anesthetic awareness when giving rocuronium before ketamine for RSI is not completely answered due to the limitations of this analysis. However, the risk is likely to be significant enough that using rocuronium before ketamine should not be routinely done. In patients with a very short estimated safe apnea time, the risk of anesthetic awareness may be less than the risk of anoxic injury and giving rocuronium first may represent the best therapeutic option for such a patient. A compatibility in syringe study of rocuronium and ketamine would be very helpful.
Do you mix ketamine and rocuronium in the same syringe? Please share and if you do mix reply w/ supporting reference if you have it!
— Pharmacy Joe ?? (@PharmacyJoe) May 1, 2017
Get CE from the podcast at pharmacyjoe.com/ce.
If you like this post, check out my book – A Pharmacist’s Guide to Inpatient Medical Emergencies: How to respond to code blue, rapid response calls, and other medical emergencies.

How about a little touch of versed given first so if you do have anesthetic awareness the patient doesn’t remember it.
Sounds reasonable. The argument made against this is that relaxing the patient first would lead to “de-recruitment” in the lungs of the morbidly obese patient in the example and further shorten the safe apnea time.
This actually happened to me, I got rocketed into aware paralysis. i am obese and sleep apnea. They gave the roconium first before ketamine and fentanyl. I had complete anesthetic awareness for at least 1- 2 whole minutes!
Worst thing thats ever happened to me. And I have a history of violent and sexual trauma and chronic pain, so thats no joke.
It was definitely a (relatively) long time because of all that happened.
I tried moving my toe. i systematically went through every muscle group. I got scared then and “threw myself” from inside several times unsuccessfully.
I went through what couldve happened wrong. Did they know I aas aware,? Was i supposed to be anesthetized? I went through everything they had said. It was not a huge rush job. They had used a nasal tube with light and let me look at vid of thrush and throat swelling too closed as i breathed ragged.
Then i tried to communicate. I tried blinking morse code, making any noise. Unsuccessfully!
Total psychic terror and desperation followed.
Thinking they accidentally paralysed me for good, or didnt know i was awake and might perform something painful on me.
Finally because i was becoming hysterical inside like spiraling rapidly towards madness, another part of me like an inner parent stepped in and said “Its ok, Rick. Close your eyes. Say your prayers and go to sleep.” So i did, crying.
I was off tube in 3 days but in hospital a wk with many issues but all i could ever tjink or talk about for weeks was those 3 minutes. I was desperate to tell anyone who would listen. The nurse explained when i woke later that 1st day and wrote about being paralyzed that it was roconium to relax throat for intubation but theyd also given me ketamine and fentanyl,. I think understanding what occurred and telling it reoeatedly helped with the trauma but i still have nightmares a year later and am considering going back into therapy because i am noticing PTS symptoms i recognize from other trauma. Now, I am a very high functioning person with alot of emotional skills. I was able to work through alot of the psychic trauma simply because I just naturally did what a therapist had previously taught me with other traumas. Most patients do not have the ability to spontaneously give themselves cognitive behavioral interventions and therapeutic self soothing.
If it had been explained to me before “there is a chance you might feel paralyzed for a minute but dont worry it goes away and you may not even remember it”
I would NOT have suffered nearly as much. I may have still been a bit scared, bit It would not have been unmitigated psychic terror and trauma.
Please TELL the patient before, during or within seconds of pushing IV rocuronium that s/he may experience this, that it is ok and normal snd will go away when sedative kicks in. PLEASE. Otherwise Its inhumane to do this to people without explanation.
Or yea if Versed is a real amnesia drug then use that too. But i dunno, the patient still experiences the psychic terror and trauma, even if s/he doesnt recall it consciously.
Trauma never really goes away without being dealt with Ive learned. Even if there is no memory its still harmful.
Thank you for reading this.
This is an outstanding analysis that fits with my experience. In very select (life-saving) scenarios, it’s worth giving the roc first, but be ready for a somewhat nasty scene for a few seconds (whether they remember it, I don’t know). I think the times where it’s warranted are relatively rare – at least, definitely not the majority)
I agree this should NOT be what we do every time – at least not with ketamine. With Etomidate or propofol, it is probabaly a different story, and giving ketamine over a minute or so does lower apnea time as well (though I am not sure about hypopnea).
I worry folks will jump on board with something like this and start to use it routinely. Might be quite a few patients with bad memories.
Thank you, great points!